Browse Business Software Categories
MEDICAL BILLING
AdvancedMD Medical Billing Review
Product Snapshot
Product Pricing
Contact vendor directly for pricing information.
Technology
Product is a SaaS solution accessible from any web-enabled browser.
Customer Focus
Vendor works with practices large and small of varying medical specialties.
Select Customers
Contact vendor directly for case studies.
Customer Case Studies
About AdvancedMD Medical Billing
 AdvancedMD offers medical billing, revenue management, and reporting solutions that help users quickly collect reimbursements and eliminate billing management complications. The AdvancedMD medical billing systems integrate with EHR software, creating a complete medical practice management solution designed to maximize collections for both single practitioners or larger provider groups. AdvancedMD assists users by integrating powerful tools like automatic claims scrubbing, one-click payment processing, and a robust clearinghouse.
AdvancedMD offers medical billing, revenue management, and reporting solutions that help users quickly collect reimbursements and eliminate billing management complications. The AdvancedMD medical billing systems integrate with EHR software, creating a complete medical practice management solution designed to maximize collections for both single practitioners or larger provider groups. AdvancedMD assists users by integrating powerful tools like automatic claims scrubbing, one-click payment processing, and a robust clearinghouse.
About the Company
AdvancedMD delivers integrated workflow and personalized service to ensure the health of every practice.
An integrated suite of cloud solutions includes practice management/medical billing, electronic health records, telemedicine, patient experience, business analytics reporting, and physician performance benchmarking all backed by expert practice advocates.
AdvancedMD also offers full-service revenue cycle management and serves an expansive national footprint of more than 22,500 practitioners across 8,000 practices and 600 medical billing companies.
AdvancedMD Medical Billing Key Features
- Online charge slips can be easily customized to a practice’s needs, workflows, and specialty
- Create customized codes for supplementary products and services
- Eliminate misplaced charge slips by using online slips
- Automatically transmit charges to in-house or outsourced billing system
- Charges are available for review as soon as they are submitted by the provider
- Review and approve charges before submission and make edits directly in the review screen
- Access a comprehensive, searchable library of the four major medical code types
- Search codes electronically by CPT and descriptions or by keywords, and then view the code details to ensure the location of the correct descriptor
- Free automatic code updates help users submit claims correctly the first time
- An intuitive interface lets front office staff check in patients in less than a minute
- Complete all check-out functions in the same screen
- Assign collection worklists to billing specialists based on criteria such as specific skills or familiarity with certain payers
- Use the automated collection worklists to divide and prioritize the workload among medical staff and increase productivity
- Set the worklists to prioritize delinquent accounts receivable in order to capture more revenue and increase overall profitabilit.
- See standard ANSI payment and denial reasons in a visual display, priovding an easy way to view, manage, and follow up on rejected claims
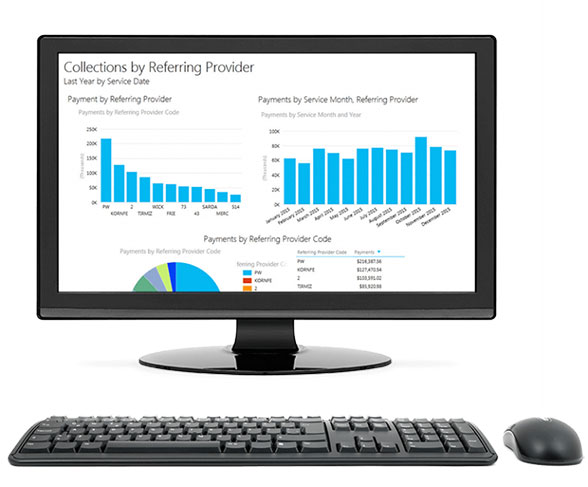
- See daily, at-a-glance updates of financial health and trends
- View revenue trends by practice location, provider, or payer
- Use templates to quickly create collection letters for the appropriate phase of the collection cycle
- Each medical collection letter can be previewed in an editing screen and modified as necessary
- Track each action and response within software system to ensure that proper follow-up and timely progressive action is take.
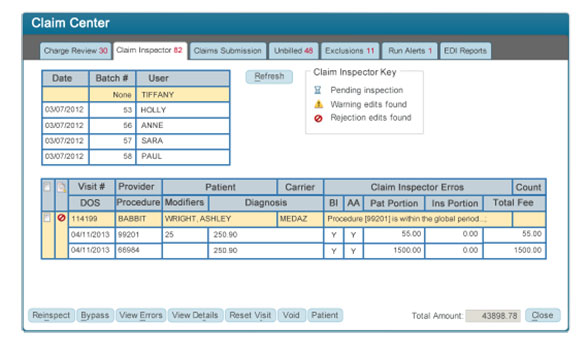
- ClaimsInspector ensures that procedures are captured correctly and claims are error-free before submitting for payment, resulting in an almost-100% first-pass claim acceptance rate
- An integrated clearinghouse helps users submit claims to hundreds of payers quickly and easily
- Resolve rejections, denials, or errors with just a few clicks, and track insurance reimbursement through final posting
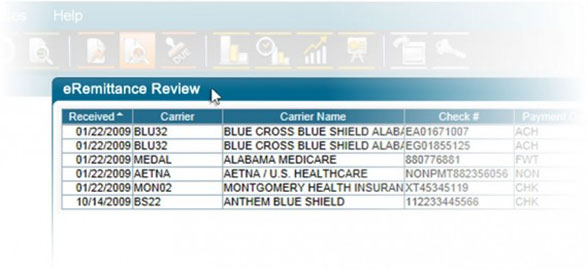
- Carrier ERAs are automatically uploaded into the eRemittance center and matched with corresponding medical visits and charges
- Integrated payment processing helps users get paid faster and saves money on third-party processing
- Payment collection is fast and easy: swipe the credit card and post the payment with a single click
- Generate daily statements for patient visits rather than waiting for a weekly or monthly batch
- Automate the entire patient billing statement process to save time and increase staff productivity
AdvancedMD Medical Billing Screenshots
White Papers and Demos
White Paper provided by AdvancedMD
Moving to ICD-10 CM/PCS will require a tremendous effort and incur incredible cost for health care organizations. Many medical organizations have not begun the implementation process and are expecting the date for implementation to be delayed. That is a misconception and could affect the health of the organization. The countdown is now. Don’t delay planning for implementation. The health of your medical organization depends on it!
White Paper provided by AdvancedMD
The best medical billing services do far more than just process claims. They follow up with insurance companies, appealing denials and working rejections, no-pays and slow-pays. They offer collaborative tools designed to boost your revenue. They manage patient payment plans. They handle monthly statement cycles. They provide solid insight into your practice’s financial health.
Products Similar to AdvancedMD Medical Billing